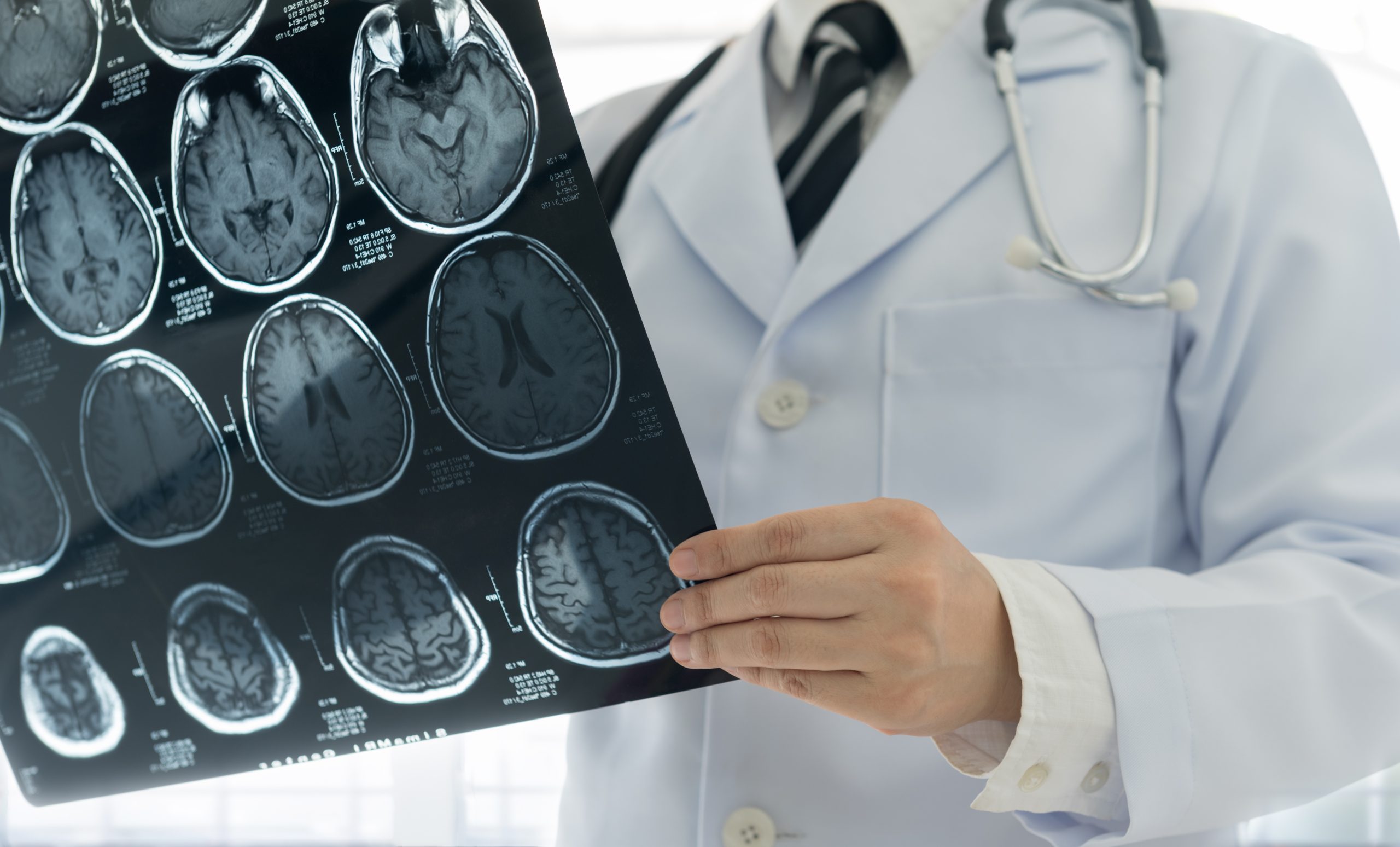
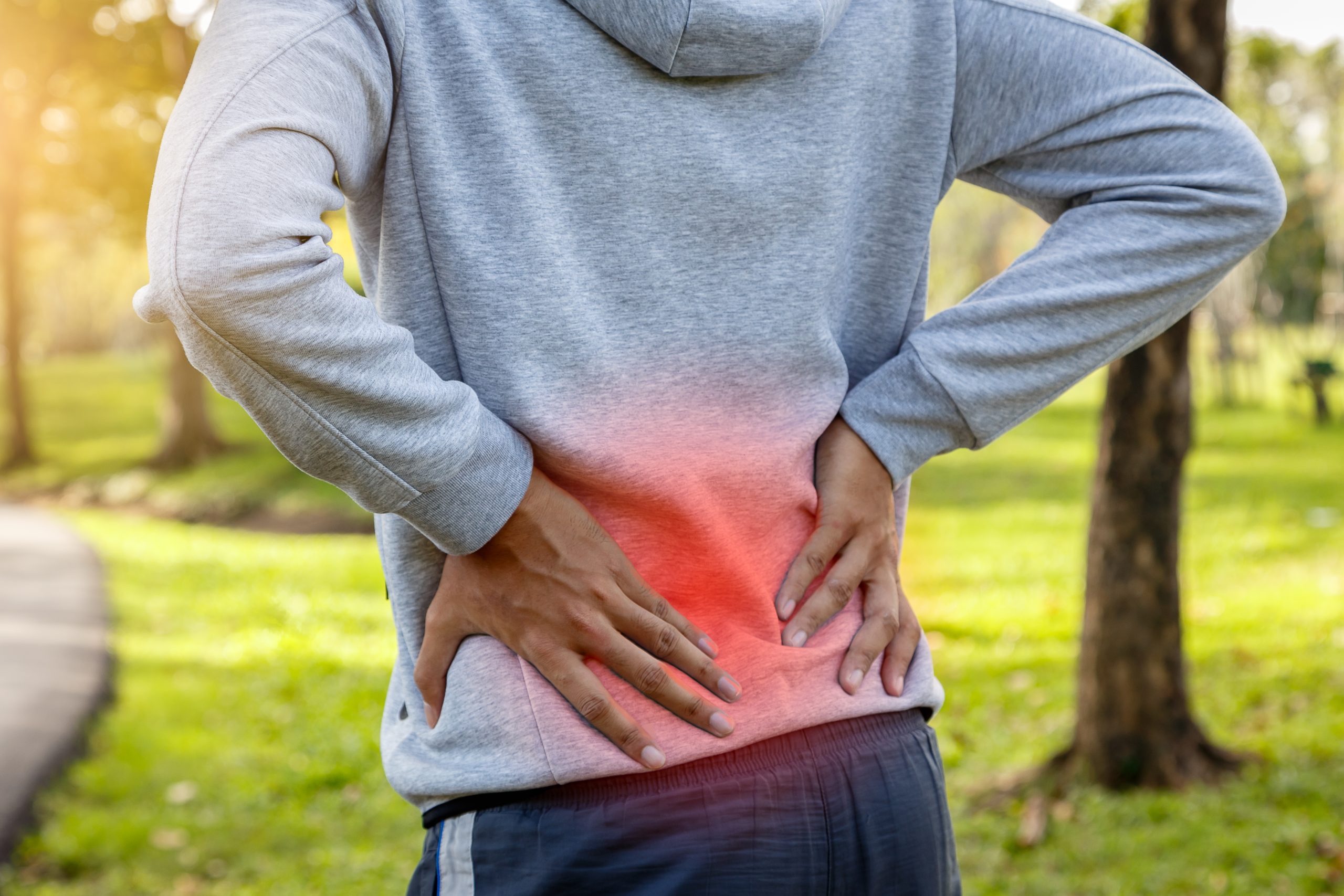
Sport man suffering from backache at park outdoors, Lower back pain concept
Findings may lead to reconsideration of how we treat acute pain
Using anti-inflammatory drugs and steroids to relieve pain could increase the chances of developing chronic pain, according to researchers from McGill University and colleagues in Italy. Their research puts into question conventional practices used to alleviate pain. Normal recovery from a painful injury involves inflammation and blocking that inflammation with drugs could lead to harder-to-treat pain.
“For many decades it’s been standard medical practice to treat pain with anti-inflammatory drugs. But we found that this short-term fix could lead to longer-term problems,” says Jeffrey Mogil, a Professor in the Department of Psychology at McGill University and E. P. Taylor Chair in Pain Studies.
The difference between people who get better and don’t
In the study published in Science Translational Medicine, the researchers examined the mechanisms of pain in both humans and mice. They found that neutrophils – a type of white blood cell that helps the body fight infection – play a key role in resolving pain.
“In analyzing the genes of people suffering from lower back pain, we observed active changes in genes over time in people whose pain went away. Changes in the blood cells and their activity seemed to be the most important factor, especially in cells called neutrophils,” says Luda Diatchenko a Professor in the Faculty of Medicine, Faculty of Dentistry, and Canada Excellence Research Chair in Human Pain Genetics.
Read the full story on the McGill University website