Injury of the spinal cord is a traumatic and life-changing event that affects over three million people worldwide. Over the last decade, researchers have been examining ways to help repair injured individuals through the use of stem cell transplantation. Significant progress has been made in this area yet many unanswered questions remain. For the laboratory of Dr. Wolfram Tetzlaff at the University of British Columbia, these gaps need to be filled to ensure successful treatments in the future.
Tetzlaff’s group has been examining spinal cord injury for years. As his team reported earlier this year in the journal, Nature Neuroscience, the concept of stem cell transplantation offers a unique chance to give the body a helping hand. But researchers and clinicians are still figuring out how to do it right.
Now his team has added even more useful information thanks to a paper published this month in The Journal of Neuroscience. They have provided a cellular map for researchers to better understand how the healing process occurs. The results also offer a new possible target for clinicians exploring transplantation therapies.
Working with mice, the team examined the microcosm of a spinal cord injury over the course of three months. This length of time is necessary to have a decent understanding of the process, which includes two phases known as subacute and chronic. His team wanted to find out how the cells within the injured area respond and possibly change over time.
During the 12 week period, Tetzlaff focused on the process in which stem cells known as oligodendrocyte precursor cells, or OPCs, produce two types of cells, oligodendrocytes and Schwann cells. For Tetzlaff, these two cell types are critical for healing. These cells help to ensure the electrical signals produced in the brain are properly sent to the rest of the body. His hope was to identify a possible place for transplantation to improve repair.
Over the three months, the team witnessed incredible changes in the injury site though many of the results were expected. Yet, there was one surprise. The formation of Schwann cells appeared to be happening at the site of injury. For Tetzlaff, this was unexpected. “Schwann cells are usually thought to be produced in peripheral nerves and then migrate to the site of spinal cord injury. While we did see this, it was minimal. Most of these cells were being produced by CNS stem cells in the injury zone, so called oligodendrocyte precursor cells, that can make more than one cell as we learned.”
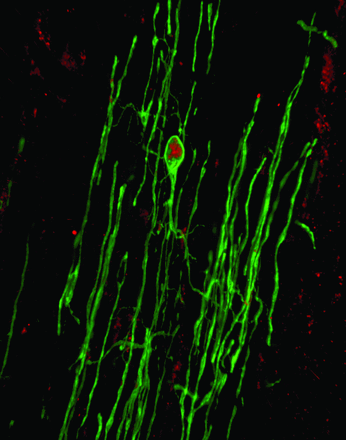
The finding was more than just an interesting observation, however. It offered a possible direction forward. Based on these results, Tetzlaff envisions how his results could potentially help to improve the success of transplants in the future. “We may be able to provide the injured area with therapies that may include the stimulation of endogenous stem cells with chemicals to increase the production of Schwann cells. This in turn can help increase the likelihood of better bridging of the spinal cord injury site.”
This study opens a new door towards possible treatment for SCI. However, more fundamental research needs to be done before this idea can be tested in humans. Tetzlaff believes this effort is necessary to help the millions who suffer. “We are getting closer to knowing how to heal spinal cord injuries but need fundamental research to fill in some of the blanks. This way, we can ensure clinicians have the best information to ensure trials end up successful and real world treatments become a reality.”
Original Research Articles:
Assinck P, Duncan GJ, Plemel JR, Lee MJ, Stratton JA, Manesh SB, Liu J, Ramer LM, Kang SH, Bergles DE, Biernaskie J, Tetzlaff W. Myelinogenic Plasticity of Oligodendrocyte Precursor Cells following Spinal Cord Contusion Injury. J Neurosci. 2017 Sep 6;37(36):8635-8654. doi: 10.1523/JNEUROSCI.2409-16.2017.
Assinck P, Duncan GJ, Hilton BJ, Plemel JR, Tetzlaff W. Cell transplantation therapy for spinal cord injury. Nat Neurosci. 2017 Apr 25;20(5):637-647. doi: 10.1038/nn.4541. Review.
